
Editorial & Legal Accuracy Notice (Louisiana)
This blog contains general legal and safety information and is not legal advice. Laws and deadlines can change, and outcomes depend on specific facts.
Last reviewed / updated: March 3, 2026
Reviewed, updated, and authored by: Stephen Babcock, Louisiana injury lawyer
This guide explains common symptoms of a broken tailbone, red flags, and how providers evaluate coccyx injuries. It also shows how to document limitations in a way that holds up in Louisiana insurance claims.
Tailbone pain after a fall or crash can be deceptively limiting because sitting, driving, and sleeping all hurt. Providers often use pattern details to decide whether you likely have a bruise, a fracture, or a joint problem. This page focuses on broken tailbone symptoms and the practical steps that keep your record clear.
Our approach is simple: we build the story from the first hour forward so the record stays consistent. We are not built for volume. We are built for leverage. Speed + evidence preservation + insurer-insider knowledge + trial-ready preparation = The Babcock Benefit. For broken tailbone symptoms, leverage means showing how pain affects function, not just pointing to a single scan.
If you are trying to link a coccyx injury to missed work or a disrupted routine, start with our orthopedic injury practice page, then use the documentation framework below. You can also print the checklists and keep them with your medical paperwork. The goal is clarity, not drama, because insurance companies look for gaps.
Firm links: Client Reviews | Contact | Locations
Download the printable toolkit (PDF) to keep the symptom tracker, evidence checklist, and both infographics in one place. It is designed for print and for sharing with your treating provider.
If you are inside the first 72 hours, call (225) 500-5000 or use the free case review form before evidence changes.
What Are the Symptoms of a Broken Tailbone?
The Cleveland Clinic’s coccydynia overview explains that tailbone pain often worsens with sitting and can flare when you move from sitting to standing. A MedlinePlus tailbone aftercare guide describes pain, tenderness, and bruising as common signs after a coccyx injury.
- Pain at the base of the spine that is worse while sitting
- Sharp pain when standing up from a chair
- Tenderness over the coccyx with pressure
- Pain during bowel movements
- Visible bruising or swelling after a fall
- Reduced sitting tolerance for driving, work, or school
One reason broken tailbone symptoms are tricky is that pain can be intense even when the injury is “only” a bruise. The same MedlinePlus guidance notes that tailbone fractures are uncommon, so many cases are contusions or sprains that still hurt when sitting. In other words, the functional limits you document often matter as much as the label.
Bruise vs. Fracture: What Changes?
Most people cannot tell at home whether they have a fracture, a bruise, or a joint alignment problem. The Merck Manual’s discussion of coccygeal injury explains that clinicians consider the mechanism, exam findings, and whether symptoms persist to determine which evaluation is needed. For claims and care, what matters is documenting the pattern and the impact on daily function.
When Should You Get Urgent Care for Tailbone Pain?
Seek urgent evaluation if tailbone pain comes with new weakness, numbness, or bowel or bladder control problems, because the American Academy of Orthopaedic Surgeons treats those symptoms as red flags for serious nerve compression. The MedlinePlus aftercare guidance also recommends calling a provider for sudden numbness or weakness and for bowel or bladder control problems after a tailbone injury.
- New trouble controlling urination or bowel movements
- Numbness in the groin or “saddle” area
- New or worsening leg weakness
- Fever or spreading redness near the area
- Severe pain after a major crash or a hard fall from height
- Pain that keeps getting worse instead of slowly improving
If you go to urgent care or the ER, be ready to describe the mechanism in a single, clear timeline sentence. The Cleveland Clinic describes evaluation as a mix of history, exam, and selective testing, so clarity helps your clinician document the right details. That documentation can also matter later if an insurer tries to characterize the injury as “just soreness.”
How Is a Broken Tailbone Diagnosed?
The Cleveland Clinic explains that clinicians often start with an exam and may use imaging like X-ray, CT, or MRI when symptoms or the mechanism call for it. In addition, the NCBI Bookshelf review on coccyx pain describes imaging as a tool used in selected cases, especially when pain persists or the cause is unclear.
| Step | What the Provider Does | Why It Matters for Care and Proof |
|---|---|---|
| History | Asks how you fell or were hit, and what makes the pain worse | Locks in the mechanism and the onset before the story drifts |
| Focused exam | Checks tenderness and looks for bruising and localized pain | Creates objective notes that match your symptom log |
| Selective imaging | Orders X-ray, CT, or MRI based on symptoms and concern level | Helps rule out other problems and documents severity when needed |
| Follow-up plan | Sets return visits, work restrictions, and symptom monitoring | Prevents “gap in care” arguments if pain continues |
Why a Normal X-Ray Does Not End It
Insurance arguments often over-focus on one “normal” study, even when pain is still limiting. The Merck Manual notes that evaluation can require specific coccygeal views, and in some cases, clinicians compare seated and standing films when instability is suspected. Practically, that means your symptom pattern and follow-up documentation may matter even if the first study is not definitive.
What Does Treatment Usually Look Like?
The Mayo Clinic’s tailbone pain guidance describes conservative care steps like activity modification, cushions, and pain control for many cases. The MedlinePlus aftercare guide also explains that bruises can improve in weeks, while fractures may take longer, which makes consistent follow-up important when symptoms persist.
- Reduce pressure: limit long sitting and use a cushion recommended by your clinician
- Use the care plan: follow medication and home-care instructions as directed
- Document function: track sitting tolerance, sleep disruption, and work limits
- Follow up: return if pain worsens, stalls, or new symptoms appear
- Keep records: save notes, restrictions, and receipts tied to the injury
If you need a time-frame reference for planning, the same MedlinePlus resource explains that a coccyx fracture can take about 8 to 12 weeks to heal, while a bruise often improves sooner. That does not mean your pain should be ignored while you “wait it out.” Instead, it is a reminder that symptoms can be meaningful long after the day of the fall.
Timeline Builder: How to Document Symptoms Day by Day
A tailbone claim is easier to evaluate when your records show a clean timeline from the incident through your daily limitations. The NCBI Bookshelf review on coccyx pain emphasizes evaluation and management that depend on the pattern over time, so your day-by-day notes help your provider document what is changing.
| Time Window | What to Write Down | What to Preserve |
|---|---|---|
| Day 0–1 | How you landed or were hit, and when the pain began | Scene photos, hazards, seat/impact photos, and incident report request |
| Day 2–3 | Triggers: sitting, stairs, driving, sleep, bowel movements | Bruising photos as it develops, appointment confirmations, receipts |
| Week 1 | Sitting tolerance (minutes), missed work tasks, and sleep interruption | Work emails/notes, employer attendance records, provider notes |
| Weeks 2–6 | What improves and what does not, plus any new symptoms | Follow-up visit notes, restrictions, and PT notes if prescribed |
This is why we push to preserve photos, reports, and timeline notes early, before repairs happen and memories blur. Evidence loss is not dramatic; it is routine, and it can affect how an insurer values a claim.

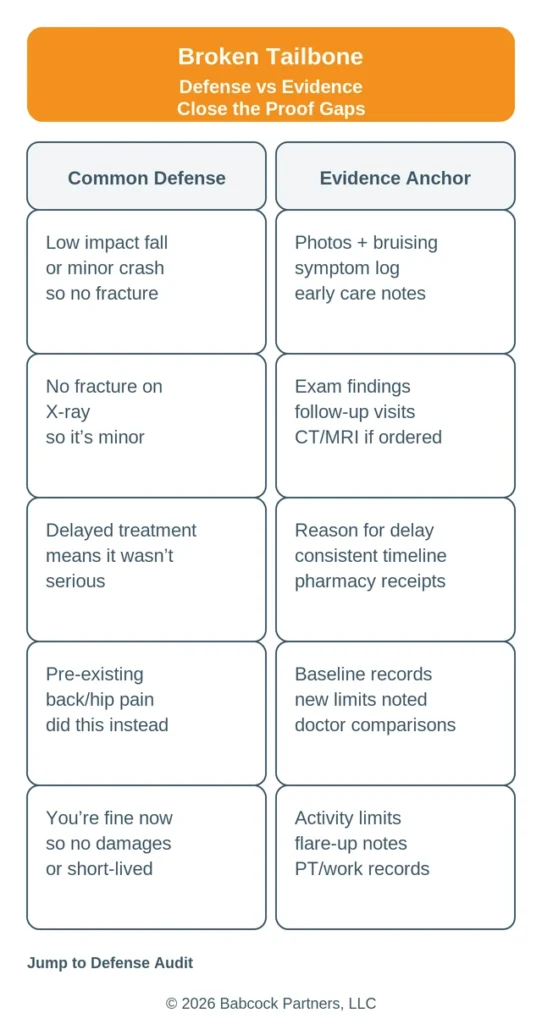
Defense Audit: How Insurance Companies Downplay Tailbone Injuries
Insurance reviews often focus on proof gaps: missing early documentation, inconsistent symptom descriptions, or a long gap between visits. The Merck Manual notes that coccygeal pain can involve different causes and evaluations, which is why insurers sometimes cherry-pick one note or one image if the record is not consistent.
| Common Defense Angle | Evidence That Counters It |
|---|---|
| “Low impact means minor injury.” | Mechanism details, scene photos, and early symptom pattern notes |
| “If it were real, you would have gone sooner.” | Appointment timeline, urgent care notes, and consistent daily logs |
| “Normal imaging means no injury.” | Exam findings, follow-up plan, and documented functional limits |
| “This is pre-existing.” | Baseline history and a clear change in function after the event |
| “You are fine now.” | Work notes, sitting tolerance tracking, and steady care cadence |
That is what we mean by leverage when we say insurers test the gaps, not just the diagnosis. If your care, notes, and timeline are consistent, the “you were fine” narrative has less room to grow.
What we see in practice
We see tailbone cases get undervalued when the record treats pain as a complaint rather than a functional limitation with a timeline. We also see insurers lean hard on gaps in care, inconsistent descriptions, and missing proof of how sitting intolerance affected work and daily life.
- Early notes say “tailbone pain,” but later notes shift to “low back pain” without explanation
- People tough it out, then the insurer claims the delay proves the injury was minor
- Imaging language gets overused, even though symptoms and exam findings can still matter
- Work and activity limits are real, but nobody documents them in a clean way
We also see problems when the first recorded statement happens before you have any medical documentation. The MedlinePlus aftercare resource highlights that symptoms and follow-up triggers can evolve, which is a good reminder not to lock yourself into an early, overconfident description. When in doubt, keep it simple and stick to what you know.
When a Broken Tailbone Is Part of a Louisiana Injury Claim
A coccyx injury often appears in claims tied to a fall, a vehicle crash, or a sudden impact to the seated area. If the event was another person’s fault, your documentation should connect the mechanism to your functional limits, and our Baton Rouge orthopedic injuries page explains how we build proof for fractures and related musculoskeletal injuries.
- Slip-and-fall incidents where the body lands seated or backward, which we discuss on our slip and fall page
- Rear-impact or sudden-stop crashes, where seated pressure spikes, which may overlap with a car accident claim
- Workplace incidents where sitting becomes a core job function problem
- Premises incidents where a hazard or a missing warning creates the fall risk
Talk to a Lawyer Quickly If
Talk to a lawyer quickly if surveillance video, incident reports, or witness information could disappear, because that proof is often time-sensitive. This is why we treat sitting limits, work restrictions, and timeline consistency as leverage, not paperwork.
Common Documentation Gaps That Hurt These Claims
The fastest way to lose leverage in a tailbone case is to leave the insurer room to redefine what happened and how it affected you. The Cleveland Clinic describes symptoms and evaluation as pattern-based, so gaps in the timeline and inconsistent descriptions are easy targets for insurance arguments.
- No early photos or incident report request, so the mechanism becomes “unclear”
- No symptom log, so sitting intolerance becomes “unproven”
- A long gap between visits, which gets framed as “you were fine”
- Work impact is real, but there are no restrictions, notes, or attendance records
- You sign a broad release before the recovery pattern is clear
Download the printable toolkit (PDF) if you want a one-page version of the timeline table and defense checklist. It is built to be used at appointments and to keep your records consistent.
Louisiana Law Snapshot (Updated 2026)
Most Louisiana injury claims have a two-year delictual prescription period, and La. Civ. Code art. 3493.1 is the starting point for understanding that deadline. Louisiana also uses comparative fault, and La. Civ. Code art. 2323 addresses fault allocation, including the post–Jan. 1, 2026 rule that can bar recovery when a claimant is 51% or more at fault.
| Rule | Plain-English Meaning | Why It Matters |
|---|---|---|
| Two-year prescription | Most personal injury deadlines run fast, and missing them can end the claim | Evidence and medical documentation need to be organized early |
| Comparative fault (51% bar after 1/1/2026) | Fault can reduce recovery, and majority fault can block it | Mechanism proof and clean timelines help avoid blame-shifting narratives |
Free Case Review: Next Steps
If you suspect a fracture or persistent coccyx pain after a crash or fall, the next step is to protect the record and move quickly before the story gets rewritten. We are not built for volume. We are built for leverage. The Babcock Benefit is our plain-English way of saying we move fast, preserve proof, and prepare the claim like it could be tried, because that changes how insurers evaluate risk.
If you want to understand your options, call (225) 500-5000 and use the free case review form to send the basics. Urgency usually comes from disappearing video, changing scene conditions, and early documentation that locks in your symptoms and work limits. If you need a starting point, review our orthopedic injuries case page and then focus on the checklist below.
These items are helpful to have with you when you call, but do not delay calling because you do not have them. If you have them handy, keep them nearby for the call.
- Date/time and location of the incident
- How you landed or what struck you, in one sentence
- Photos of the scene and any visible bruising
- Your symptom log and sitting tolerance notes
- Provider list, visit dates, and any work restrictions
Call Today If
- You are within 72 hours and video or reports may disappear
- You were asked for a recorded statement or quick settlement
- You have new numbness, weakness, or bowel/bladder symptoms
- Your job depends on sitting or driving and you cannot do it
- Your pain is not improving and you are unsure what to do next
What Happens Next
- Evidence triage: we identify what can disappear and how to preserve it
- Deadline spotting: we map legal and insurance deadlines that affect leverage
- Insurer contact strategy: we protect you from bad-record traps and control the first narrative


