Editorial & Legal Accuracy Notice (Louisiana)
This blog contains general legal and safety information and is not legal advice. Laws and deadlines can change, and outcomes depend on specific facts.
Last reviewed / updated: March 2, 2026
Reviewed, updated, and authored by: Stephen Babcock, Louisiana injury lawyer
This guide explains how long-term traumatic brain injury (TBI) symptoms are documented and why proof can be harder than people expect. It also outlines evidence steps and Louisiana deadlines that can affect legal rights.
If you are inside the first 72 hours, call (225) 500-5000 or use the free case review form before evidence changes.
Firm links: Client Reviews | Contact | Locations
Download the printable toolkit (PDF) to keep the proof steps and checklists in one print-friendly handout. The PDF includes both infographics in a clean layout.
What Are the Long-Term Effects of a Traumatic Brain Injury?
NIH’s National Institute of Neurological Disorders and Stroke explains that traumatic brain injury (TBI) can affect thinking, movement, sensation, and emotional functioning, and those effects can persist. Long-term problems often look like changes in memory, attention, sleep, mood, balance, and stamina that show up most at work, school, and home.
- Cognitive: memory lapses, slowed thinking, trouble focusing
- Physical: headaches, dizziness, fatigue, light/noise sensitivity
- Sleep: insomnia, oversleeping, unrefreshing sleep
- Mood: irritability, anxiety, depression symptoms
- Balance/vision: vertigo, blurred vision, motion sensitivity
- Function: missed work, reduced hours, mistakes, safety concerns
Mayo Clinic’s traumatic brain injury overview notes that symptoms can include thinking and behavior changes, not just physical pain, which is why “I can walk” is not a full recovery test. If you are trying to understand the legal side, start with the documentation steps in our Baton Rouge brain injury lawyer page and then use the sections below to build your proof file.
Can TBI Symptoms Show Up Later or Get Worse?
The CDC’s signs-and-symptoms overview explains that mild TBI and concussion symptoms can involve thinking, sleep, physical, and mood changes, and they can evolve after the initial event. It is common for people to feel “off” when they return to normal life demands like screens, driving, or work schedules.
- Delayed recognition: symptoms stand out once adrenaline fades
- Symptom flares: headaches or dizziness spike with activity
- Sleep disruption: poor sleep makes thinking symptoms worse
- Mood shift: irritability or anxiety grows with stress
- Work problems: mistakes, slow processing, missed deadlines
Mayo Clinic’s post-concussion syndrome page describes how symptoms can last for weeks or months in some people, especially when sleep and stress are not under control. This is why we recommend a simple daily log that tracks symptoms, triggers, and missed activities, because it creates a clean “before/after” picture when memories blur.
Does a Normal CT or MRI Rule Out a TBI?
The CDC’s mild TBI and concussion overview explains that a brain scan is not required to diagnose a mild TBI, and imaging is often used to look for dangerous complications rather than “prove” a concussion. Merck Manual’s concussion guide notes that CT and MRI results are usually normal in concussion, so symptom history and exam details matter.
- Normal scan: does not automatically mean normal brain function
- What matters: consistent symptoms, exams, and follow-up notes
- Better proof: testing that measures attention, memory, balance, or vision
- Risk issue: scans can still be urgent if red-flag symptoms appear
Insurance adjusters often lean hard on “normal imaging” because it sounds simple, even when the day-to-day function story is not simple at all. That is what we mean by leverage when we build a record that shows consistent complaints, consistent care, and objective testing instead of debating one scan report.
What Testing and Follow-Up Care Help Document a TBI?
Cleveland Clinic’s traumatic brain injury overview explains that evaluation and recovery planning can involve symptom review, neurologic exams, and referrals based on what is affected. Johns Hopkins Medicine’s TBI guide describes a range of care needs, which is why follow-up documentation often matters more than a single ER visit.
| Testing or Care Step | What It Helps Document | Practical Evidence Tip |
|---|---|---|
| Neurologic exam + symptom history | Pattern and persistence of cognitive, balance, and mood complaints | Bring a short written list of symptoms and triggers to every visit |
| Vestibular/ocular screening | Dizziness, motion sensitivity, visual tracking issues | Ask for the test name in the note so it is easy to find later |
| Neuropsychological testing | Attention, memory, processing speed, executive function | Keep school/work examples that match the deficits found |
| Therapy and rehab records | Functional limits and progress over time | Save attendance records and home exercise instructions |
| Primary care follow-up | Consistency of complaints and referrals | Follow the referral chain when symptoms continue |
MedlinePlus explains that traumatic brain injury can range from mild to severe and that follow-up needs vary, which is why the “right test” depends on what is actually impaired. If your main issue is attention, balance, or sleep, documentation should match the problem instead of forcing a one-size-fits-all approach.
Timeline Builder: How Do You Prove What Changed?
You prove long-term traumatic brain injury (TBI) effects by building a clean, dated story that starts with the event and ends with specific daily-life limitations. The goal is not to be dramatic; the goal is to be consistent, because insurers look for gaps and contradictions.
- Start with the event: where you were, what happened, and who saw it
- Mark first symptoms: headache, dizziness, fog, sleep problems, mood shift
- Track function changes: missed work, mistakes, slower reading, unsafe driving
- Log care: ER, follow-ups, referrals, therapy, testing dates
- Keep a simple “now” snapshot: what you can’t do the same way

First 72 Hours: Evidence That Can Disappear
The first 72 hours matter because digital and third-party records can vanish or become harder to retrieve, even while your symptoms are still developing. Quick preservation steps can keep the “what happened” evidence separate from the later medical story.
- Video: nearby businesses, doorbells, dash cams, rideshare footage
- Vehicle data: photos of damage, repair estimates, event data when available
- Witnesses: names, numbers, and a short description of what they saw
- Digital trail: missed shifts, calendar cancellations, messages about symptoms
- Your notes: first symptoms, triggers, and what made you stop an activity
This is why we focus on evidence preservation early, before an insurer can argue that missing video or missing witnesses means the crash “must not have been serious.” If you are in Baton Rouge, you can also review local resources and service areas through the Baton Rouge hub page while you gather documentation.
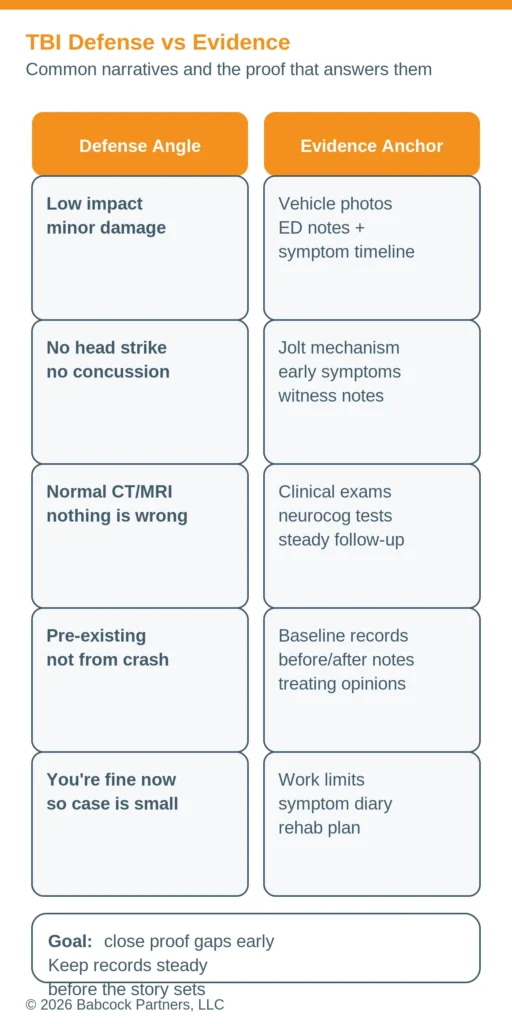
Defense Audit: Common TBI Arguments and Counters
Insurance defenses in traumatic brain injury (TBI) cases usually focus on a simple narrative: the crash was minor, the scans were normal, and your symptoms come from something else. You can counter that narrative by matching each defense angle with a specific, dated record anchor.
| Common Defense Angle | Evidence Anchor That Helps |
|---|---|
| “Low impact” or “minor damage” | Scene photos, repair records, witness descriptions, early symptom timeline |
| No head strike, so no TBI | Mechanism explanation (jolt), first symptoms, consistent follow-up notes |
| Normal CT/MRI means you are fine | Clinical exam findings, neurocognitive or vestibular testing, steady care |
| Pre-existing issues caused this | Baseline records, clear before/after function change, treating provider notes |
| You seem fine now | Work/school limits, symptom diary, therapy notes, relapse triggers |
What we see in practice
In long-term TBI cases, we usually see two battles happening at once: the medical battle to stabilize symptoms and the paperwork battle to prove impact over time. The paperwork battle is often lost in the small details, like inconsistent symptom language or missing work documentation.
- Early “I’m okay” statements get repeated later as if they were a final diagnosis
- Gaps in care get framed as “you must have felt fine” instead of real life logistics
- Normal imaging gets treated like the case is over, even when function changed
- Pre-existing history gets overstated unless baseline records are collected
- Work and school proof gets overlooked even though it is often the clearest impact
Documentation Strategy: Make Symptoms Verifiable
Good TBI documentation turns “I feel off” into dated examples that a doctor can chart and an insurer can’t dismiss as vague. The key is consistency: the same symptoms, described the same way, tracked over time.
- Use a 1-page symptom log: date, trigger, symptom, recovery time
- Bring examples: missed appointments, errors at work, unsafe driving moments
- Ask for specifics in notes: balance tests, cognitive screens, vision findings
- Document accommodations: reduced hours, extra breaks, screen limits
- Save receipts: therapy, prescriptions, rides, help at home
The CDC’s symptom list for concussion and mild TBI highlights how wide-ranging these issues can be, which is why a scattered record can look contradictory when it is really incomplete. If you post on social media, be careful with “I’m fine” updates that do not match your medical complaints, because insurers often look for statements they can quote.
When Should You Talk to a Louisiana TBI Lawyer?
If a traumatic brain injury is affecting work, driving, sleep, or relationships, it is smart to talk to a lawyer before the insurance narrative hardens and before records go missing. Louisiana Civil Code article 2315 is the basic fault rule for personal injury, and a claim usually rises or falls on proof of fault, causation, and damages.
- Early red flags: worsening headaches, confusion, vomiting, or new neurologic symptoms
- Proof red flags: no photos, no witness info, or delayed care with no explanation
- Insurance red flags: pressure for a recorded statement or a fast release
- Work-life impact: missed shifts, mistakes, reduced hours, or accommodations
- Complex crashes: commercial drivers, multiple vehicles, or unclear fault
If your TBI started after a wreck, our team can help you organize documentation and next steps through traumatic brain injury (TBI) claim help while keeping the scope focused on the injury proof. If your main question is the crash itself, we cover accident-side issues on the Baton Rouge car accident page.
Common Mistakes That Hurt Long-Term TBI Proof
Most long-term TBI cases do not fail because the symptoms are not real; they fail because the record looks inconsistent or incomplete. A few small choices in the first weeks can make later proof much harder.
- Skipping follow-up: letting weeks pass with no documented complaints
- Changing symptom language: “fine” in one visit and “severe” in the next with no context
- Underreporting: not mentioning sleep, mood, or vision issues because they feel “non-medical”
- Overdoing activity: triggering flares without noting what caused them
- Signing too early: agreeing to a release before the symptom pattern stabilizes
If you want a single-page reference, Download the printable toolkit (PDF) before your next appointment. It includes a symptom log template and the defense-vs-evidence checklist.
Louisiana Law Snapshot (Updated 2026)
Louisiana Civil Code article 3493.1 sets a two-year delictual prescription period for many injury claims, which means waiting can risk losing the right to file. Louisiana Civil Code article 2323 covers comparative fault, and for claims governed by the post–Jan. 1, 2026 rule, recovery can be barred if the plaintiff is 51% or more at fault.
- Do not wait for “final symptoms” before preserving evidence and documenting care
- Fault questions matter early because comparative fault can reduce or bar recovery
- Deadlines can be tricky in multi-party crashes, commercial cases, or unclear identity cases
If you think a deadline issue exists, it is safer to talk to a lawyer quickly and confirm the calendar than to assume you have time. Evidence preservation can also start before you know every medical answer.
Free Case Review: Protect the Record
We are not built for volume. We are built for leverage. In a long-term traumatic brain injury (TBI) claim, the Babcock Benefit means moving fast on proof and then preparing the file like it may be tried. If you want to see how we handle brain injury cases, start with our brain injury case approach and then call (225) 500-5000 or use the free case review form.
Acting early matters because video and witness details fade, symptoms can fluctuate, and insurers often lock onto a “normal scan” narrative quickly. Even if you are still figuring out treatment, you can preserve the evidence that later supports the medical story.
These items are helpful to have with you when you call, but do not delay calling because you do not have them. If you have them handy, keep them nearby for the call.
- Crash or incident date, location, and any report number
- A short symptom list and the biggest daily-life limitations
- Provider names and visit dates (ER, primary care, specialists, therapy)
- Photos, video links, and witness contact information
- Insurance claim number and adjuster contact, if available
Call today if any of these apply because proof and deadlines tend to move faster in these situations. It is easier to preserve evidence now than to rebuild it later.
- You are being pushed to give a recorded statement or sign a release
- Your symptoms are worsening, changing, or interfering with work or driving
- A commercial vehicle or multiple vehicles were involved
- Video may exist but could be overwritten soon
- You have a prior head injury history that may be used against you
What happens next is practical and focused on leverage, not hype. We triage evidence, spot deadlines, and control insurer communications so the record stays consistent.
- Evidence triage: identify what can disappear and preserve it first
- Deadline spotting: confirm the correct filing deadline and key notice issues
- Insurer contact strategy: keep communications consistent with the medical story


